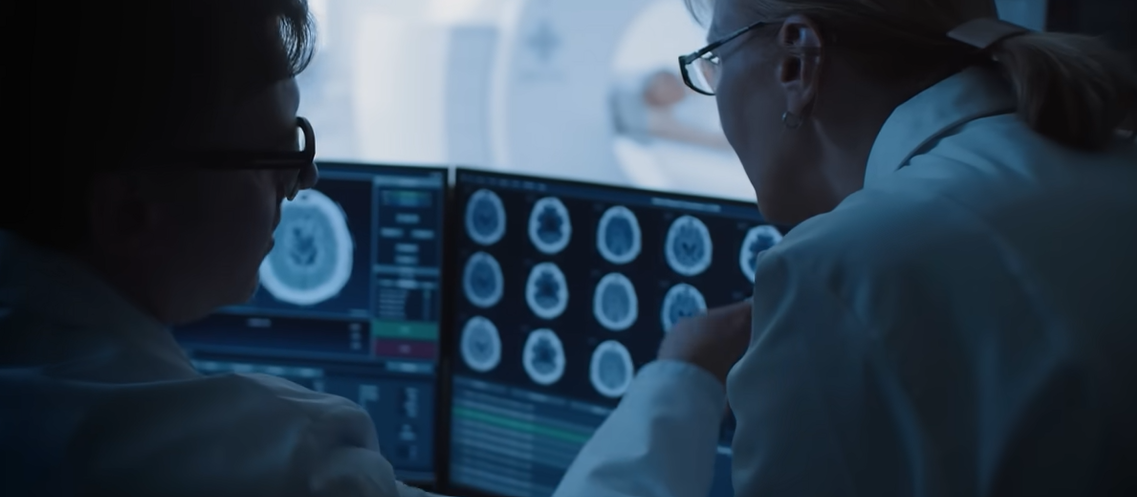
In the field of medicine, artificial intelligence has evolved from an experimental instrument to a highly productive clinical collaborator. AI is now able to precisely scan thousands of MRIs and X-rays in radiology labs, which has significantly increased the rates of early cancer detection. Treatments can begin days or weeks earlier thanks to these systems, which detect minute irregularities that even experienced specialists might miss. This difference can save lives. The technology analyzes continuously without getting tired or distracted, functioning almost like an exceptionally clear second opinion.
AI is especially inventive in drug research. Algorithms can sort through millions of compounds in a matter of weeks, whereas conventional techniques might take years to find a promising molecule. For instance, DeepMind’s AlphaFold has significantly accelerated the comprehension of protein structures, changing the process of creating new medications. Giants in the pharmaceutical industry are embracing these innovations not only to expedite the process but also to develop highly targeted treatments that lower side effects and greatly increase patient recovery rates.
AI’s capacity to combine genetic data with current health information has greatly aided personalized medicine. AI systems can anticipate medical flare-ups before symptoms manifest by utilizing wearable technology, continuous glucose monitors, and electronic health records. The management of chronic illnesses has benefited greatly from this type of preventive care, which provides interventions that keep patients out of hospitals and improve their daily health. It’s similar to having a performance coach who is always improving every move for someone like an athlete recuperating from an injury.
AI in Medicine and Healthcare — Key Facts
| Category | Details |
|---|---|
| Field | Artificial Intelligence in Healthcare |
| Key Applications | Diagnostics, Personalized Medicine, Drug Discovery, Treatment Optimization, Workflow Automation, Remote Patient Monitoring |
| Notable Technologies | Machine Learning, Deep Learning, Natural Language Processing, Rule-based Expert Systems |
| Leading Innovators | IBM Watson Health, Google DeepMind, Microsoft Healthcare, Apple Health, Amazon Comprehend Medical |
| Industry Value | $11B (2021) projected to $187B by 2030 |
| Benefits | Improved accuracy, faster diagnoses, reduced costs, personalized care, extended access to rural areas |
| Challenges | Data privacy, algorithmic bias, ethical concerns, regulatory compliance, physician trust |
| Societal Impact | Potential to reduce healthcare disparities, improve patient outcomes, and lower systemic costs |
| Global Trends | Rapid adoption in diagnostics, imaging, predictive analytics, and virtual health assistants |
| Reference | www.foreseemed.com/artificial-intelligence-in-healthcare |
Despite being less glamorous, administrative efficiency is very effective at freeing up medical personnel. Complex transcription tasks can now be handled by natural language processing tools, which instantly convert spoken consultations into structured records. Algorithms for scheduling appointments pair clinician availability with patient urgency, which lowers wait times and raises patient satisfaction. These tools become extremely versatile in clinics with a shortage of staff, allowing teams to concentrate on the human elements of care that machines cannot duplicate.
There are still obstacles in spite of the momentum. The consequences of algorithmic bias can be dangerously unequal if models are trained on small datasets. An AI risk assessment tool in the United States was found to recommend less care for Black patients than for white patients with comparable needs in a widely publicized case. This pattern is remarkably similar to long-standing systemic problems in healthcare. To close these gaps, thorough testing, a variety of data sources, and open supervision are required.
Data privacy is yet another important factor. Because medical records are sensitive, AI developers must create incredibly dependable encryption and storage systems. Once viewed with suspicion, cloud collaborations between technology firms and health systems are now proving crucial for striking a balance between patient trust and innovation. Robust regulatory frameworks, such as those being developed by the FDA and the European Union, are starting to establish the moral guidelines for this new era.
The most human obstacle is probably physician acceptance. Although many medical professionals agree that AI has the potential to improve decision-making, they are wary of relying too much on it. The AI-assisted diagnostics trials at Harvard Medical School show a balanced strategy: the algorithm makes suggestions, but the clinician makes the final choice, maintaining context and accountability.
The story of international adoption is captivating. Patients in the UK can begin potentially life-saving treatments sooner thanks to the NHS’s use of AI, which reduces radiotherapy preparation times by up to 90%. AI-powered diabetic retinopathy screening devices in rural India identify conditions that could endanger vision in areas without local eye specialists. Through basic voice and image analysis, mobile AI apps help local health workers diagnose pediatric pneumonia throughout Africa. When compared to manual assessments alone, these efforts are noticeably better, faster, and more accurate.
Collaboration is becoming just as crucial as competition as the industry rushes toward its estimated $187 billion valuation. Modeled after the historic collaboration during the COVID-19 vaccine race, public-private data-sharing initiatives could hasten AI’s impact in addressing other urgent health emergencies. AI-enabled global health networks in the future might support a movement toward universal preventive care by using patient data that has been anonymized.
There may be significant societal advantages. Predictive healthcare has the potential to alleviate the burden on overworked systems, especially in areas with acute shortages of medical personnel. Consider a remote clinic with AI tools that can identify heart conditions early and refer only the most serious cases to hospitals in the city. In addition to saving money, this would also save lives, time, and energy.
In the end, AI in healthcare aims to enhance physicians’ skills rather than replace them. The goal is to change reactive medicine into precision-driven, proactive care. AI broadens a doctor’s perspective into previously unobserved facets of patient health, much like the stethoscope did in the past. If this collaboration between machine intelligence and human intuition is successful, medicine may become more efficient, equitable, and compassionate than it has ever been.